What is Sarcoma?
Sarcoma can form anywhere in the body at any age.
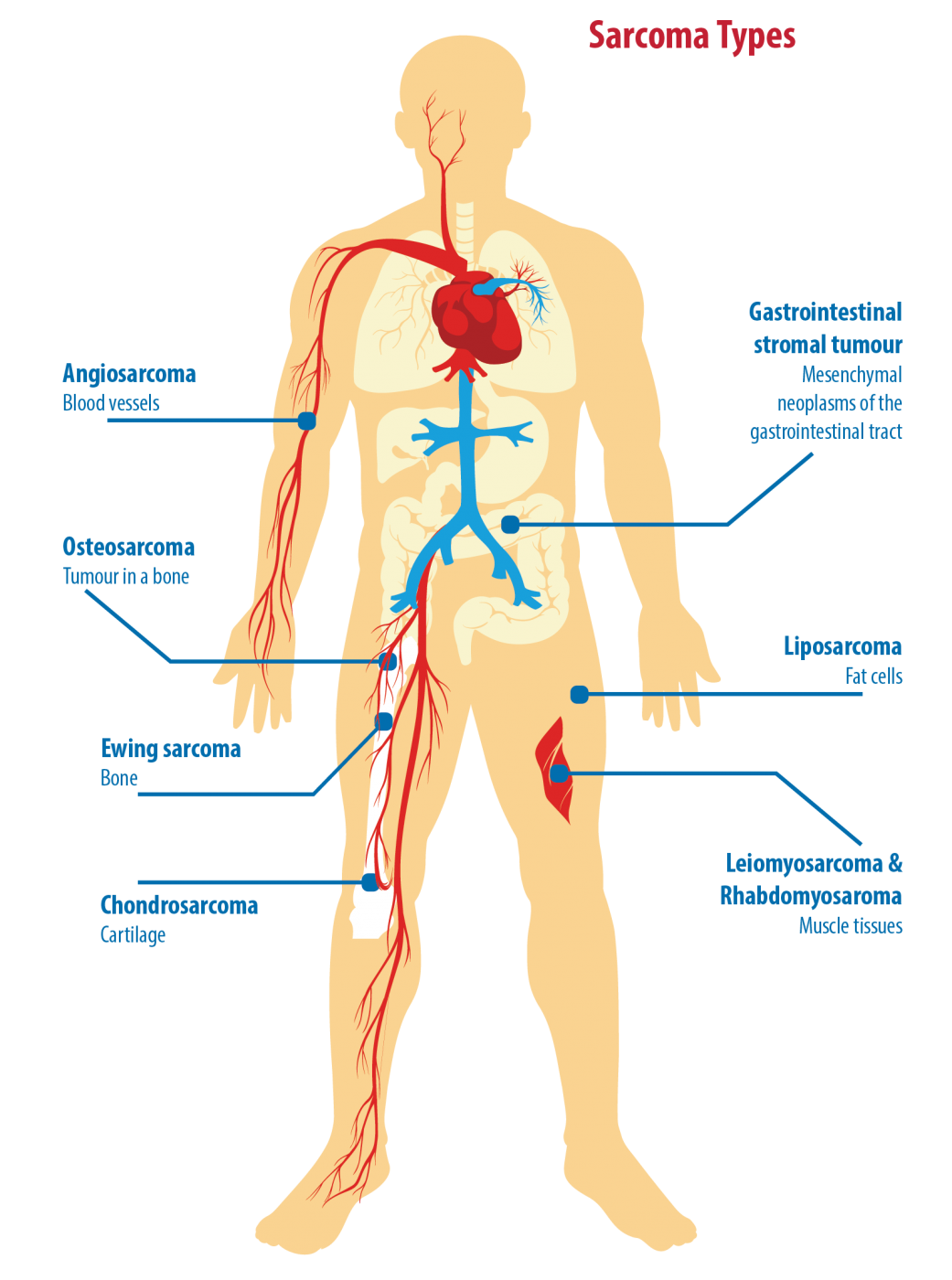
Sarcoma is a rare and complex cancer (malignant tumour) arising from the bone, cartilage or soft tissues such as fat, muscle, connective tissue or blood vessels.
Sarcomas can form anywhere in the body and are frequently hidden deep in the limbs. They are often misdiagnosed as a benign (non-cancerous) lump, or as a sporting injury or growing pains in young people.
There are more than 80 different subtypes of sarcoma, many of which have distinct clinical characteristics with unique natural history and tumour biology.
Prevalence
- Sarcoma makes up only 1% of all adult cancers.
- Sarcoma accounts for about 20% of cancers diagnosed in childhood, making it one of the most common cancers in children.
- Sarcoma makes up to 10% of cancers among adolescent and young adults (aged 15-25).
Mortality
- The 5-year survival rates for adults and children with bone and soft tissue sarcomas are estimated at 70% and 67% respectively. This depends on the extent of disease at diagnosis (e.g. stage), the tumour characteristics (e.g. some sarcomas are more aggressive than others in spreading) and response to treatment.
- While the 3-5 years overall survival rate has improved over the decades thanks to research, survivorship issues after completion of treatment, limited therapy options beyond the first-line therapy and poor outcome for metastatic sarcoma remain challenging problems to address.
Download our sarcoma fact sheet as a useful resource.
Soft Tissue Sarcoma
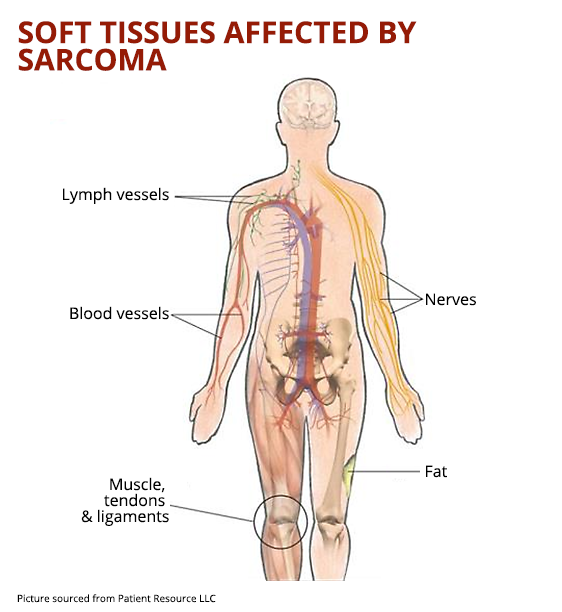
Soft tissue sarcoma is a rare type of sarcoma that develops in connective tissues such as fats, muscles, nerves, deep skin tissues and blood vessels. These tissues support and connect all the organs and structures of the body.
Usually forming first as a painless lump (tumour), soft tissue sarcoma is most commonly developed in the thigh, shoulder and pelvis. Sometimes they can grow in the abdomen or chest (trunk).
Subtypes of Soft Tissue Sarcoma
There are over 70 different subtypes of soft tissue sarcoma and they are named after the abnormal cells that make up the sarcoma.
Most common subtype of soft tissue sarcoma include:
- Undifferentiated pleomorphic sarcoma (previously known as malignant fibrous histiocytoma) from abnormal spindle-shaped cells
- Liposarcoma from fat tissue
- Leiomyosarcoma and Rhabdomyosarcoma from muscle tissues
- Angiosarcoma from blood vessels
- Malignant Peripheral Nerve Sheath Tumour (MPNST or PNST)
- Gastrointestinal Stromal Tumour sarcoma (GIST) (this is treated differently from other types of soft tissue sarcoma)
- Synovial sarcoma
Causes
Cancer occurs when cells multiply uncontrollably, forming growths called tumours. While the causes of most sarcomas are generally unknown, there are several risk factors.
Risk Factors
Factors that may increase a person’s risk of soft tissue sarcoma include:
- Radiotherapy
- There is a very small risk for people who've had radiotherapy. The risk is higher for people who had high doses of at a very young age. However, most people who have had in the past won't develop a sarcoma.
- Inherited syndromes
- A risk of soft tissue sarcoma can from your parents.
- syndromes that increase your risk include hereditary retinoblastoma, Li-Fraumeni syndrome, familial adenomatous polyposis, neurofibromatosis, tuberous sclerosis and Werner syndrome.
- Chemical exposure
- Exposure to certain chemicals, including vinyl chloride, dioxins and herbicides, has been associated with increased rates of soft tissue sarcomas.
Symptoms
Soft tissue sarcomas often have no obvious symptoms in the early stages, but can cause symptoms as they get bigger or spread. The symptoms depend on where the cancer develops.
You should see your GP if you have a worrying lump – particularly one that is getting bigger over time or is the size of a golf ball or larger – or any other troublesome symptoms.
Although it is much more likely you have a non-cancerous condition, such as a cyst (fluid under the skin) or lipoma (fatty lump), it's important to get your symptoms checked out.
Diagnosis
If your GP feels there's a possibility you have cancer, they'll refer you for a number of hospital tests.
Diagnosis for soft tissue sarcoma will usually be made by a health specialist and will be based on your symptoms, physical examination and the results of:
- Scans – an ultrasound scan is the first test performed and is ; further scans such as computed tomography (CT) and magnetic resonance imaging (MRI) scans may later.
- Biopsy – a sample of suspected cancerous tissue is removed using a needle during an operation, so it can be tested and analysed in a laboratory.
If a diagnosis of a soft tissue sarcoma is confirmed, a pathologist will further examine how likely the cancer is to spread (known as grade), and whether or how far the cancer has spread (known as stage).
Treatment
People with a soft tissue sarcoma are cared for by a multi-disciplinary team (MDT) of health specialists (usually pathologists, radiologists, surgeons, radiation oncologists, medical oncologists and paediatric oncologists), who will help decide on the most appropriate treatment.
Treatment decision depends on factors such as the tumour location, the subtype of sarcoma, how far it has spread, age and general health.
The main treatments are:
- Surgery – removing any tumour is the treatment for most types of soft tissue sarcoma.
- Radiotherapy – the use of high-energy radiation to kill cancer cells.
- Chemotherapy – the use of anti-cancer drugs to kill cancer cells.
These treatments can be given alone or in combination.
Information sourced from:
- Cancer Council Victoria - https://www.cancervic.org.au/cancer-information/types-of-cancer/soft_tissue_cancers/soft-tissue-cancers-overview.html
- Kick Sarcoma - https://kicksarcoma.org.sg/what-are-sarcomas/types-of-sarcomas/
- NHS - https://www.nhs.uk/conditions/soft-tissue-sarcoma/
- Mayo Clinic - https://www.mayoclinic.org/diseases-conditions/soft-tissue-sarcoma/symptoms-causes/syc-20377725
- The Liddy Shriver Sarcoma Initiative - http://sarcomahelp.org/sarcoma-treatment.html#tpm1_3
- Australian Institute of Health and Welfare - https://www.aihw.gov.au/reports/cancer/cancer-data-in-australia/contents/survival
Bone Sarcoma
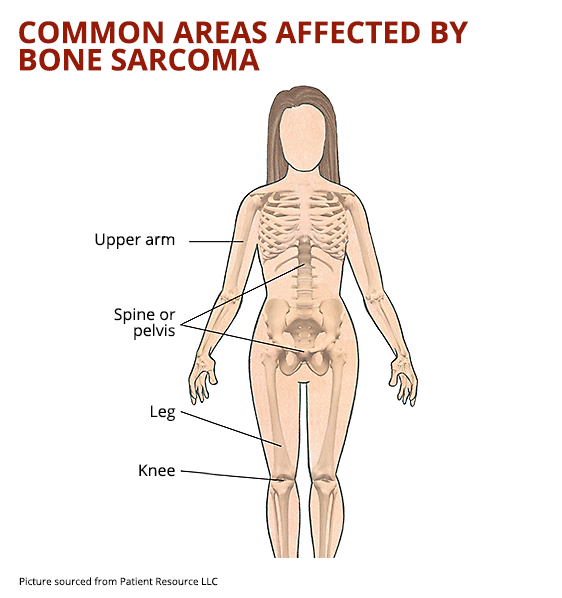
Bone sarcoma is a rare type of cancer that arises from bone and cartilage, commonly presenting with a painful lump (tumour) in limbs. The most common places where bone sarcoma develops are around the knee, wrist, shoulder and pelvis.
About 200 Australians are diagnosed with bone sarcoma each year; and is more common among children, youth and young adults.
Bone sarcoma is different from secondary bone cancer, which is cancer that spreads to the bones after developing in another part of the body.
Subtypes of Bone Sarcoma
Three most common types include:
- Osteosarcoma (accounts for about 35% of bone sarcoma)
- Starts in cells that grow bone.
- Often affects the arms, legs and pelvis, but may occur in any bone.
- More commonly affects children, adolescents and young adults within growing bones; and older people in their 70s and 80s.
- Osteosarcoma as high-grade tumours.
- Chondrosarcoma (accounts for about 30% of bone sarcoma)
- Starts in cells that grow cartilage.
- Often affects the bones in the upper arm and legs, pelvis, ribs and shoulder blade.
- More commonly affects people aged over 40.
- Chondrosarcoma as low-grade tumours – a slow-growing form of cancer that rarely spreads to other parts of the body.
- Ewing sarcoma (accounts for about 15% of bone sarcoma)
- Affects cells in the bone or soft tissue that rapidly and often have a large lump associated with it.
- Often affects the pelvis, legs, ribs, spine and upper arms.
- It is more common among children, youth and young adults, but it can occur at any age.
- Ewing sarcoma as high-grade tumours.
Causes
While the causes of most bone sarcomas are unknown, however, there are several risk factors.
Risk Factors
Factors that may increase a person’s risk of bone sarcoma include:
- Previous radiotherapy, particularly for people who received high doses at a young age.
- Other bone conditions such as Paget's disease of the bone, fibrous dysplasia or multiple enchondromas.
- Genetic factors such as inherited conditions like Li-Fraumeni syndrome, and a strong family history of certain cancers.
Symptoms
The most common symptom of bone sarcoma is a pain in the bones and joints. The pain gradually becomes constant and does not improve with mild pain-relieving medicines. It may be worse at night or during activity.
Other symptoms can include:
- Swelling over the affected part of the bone.
- Stiffness or tenderness in the bone.
- Problems with movement such as an unexplained limp
- Loss of feeling in the affected limb
- A fractured bone
- Unexplained weight loss
- Fatigue
Most people who have these symptoms do not have bone sarcoma. If you have symptoms for more than two weeks, you should see your GP.
Diagnosis
If your GP feels there's a possibility you have cancer, they'll refer you for a number of hospital tests.
Diagnosis for bone sarcoma will usually be made by a health specialist and will be based on your symptoms, a physical examination and the results of:
- Scans – X-rays, magnetic resonance imaging (MRI), positron emission tomography (PET) or computed tomography (CT) scans are usually the first of diagnosis.
- Bone biopsy – a sample of suspected cancerous tissue is removed, using a needle or during an operation it can be tested and analysed in a laboratory.
If a diagnosis of a bone sarcoma is confirmed, a pathologist will further examine how likely the cancer is to spread (known as grade), and whether or how far the cancer has spread (known as stage).
Treatment
Osteosarcoma and Ewing sarcoma are treated with multimodality (combination) approach including chemotherapy, surgery and/or radiotherapy. Chondrosarcoma is generally managed with surgery alone.
- Surgery
- Limb-sparing surgery – taking out and a margin of healthy tissue while still keeping your limb.
- Amputation – sometimes it is not possible to remove all without affecting the arm or leg. In these cases, the health specialist may advise that the only effective treatment will be to remove the limb. However, this is becoming less common with the improvement limb-sparing surgery.
- Radiotherapy uses high-energy radiation to kill cancer cells.
- Chemotherapy – the use of anti-cancer drugs to kill cancer cells.
Information sourced from:
- Cancer Council Victoria - https://www.cancervic.org.au/cancer-information/types-of-cancer/bone_cancer/primary-bone-cancer-overview.html
- Kick Sarcoma - https://kicksarcoma.org.sg/what-are-sarcomas/types-of-sarcomas/
- NHS - https://www.nhs.uk/conditions/bone-cancer/
- Mayo Clinic - https://www.mayoclinic.org/diseases-conditions/bone-cancer/symptoms-causes/syc-20350217
- The Liddy Shriver Sarcoma Initiative - http://sarcomahelp.org/sarcoma-treatment.html#tpm1_3
- Australian Institute of Health and Welfare - https://www.aihw.gov.au/reports/cancer/cancer-data-in-australia/contents/survival